Our methods of cell therapy that have successfully passed clinical application:
Primary Cell – an innovative technique of cell therapy of somatic diseases with their own regenerative cells removed from adipose tissue at the stage of early passage.
Natural rejuvenation at the cellular level makes it possible to correct immunological disorders, improve tissue trophism and blood supply, and thus restore the body’s regenerative capacity.
The technology involves the extraction and isolation of stem cells from the patient’s own adipose tissue with the subsequent stage of washing and selective choice of cells with high regenerative potential.

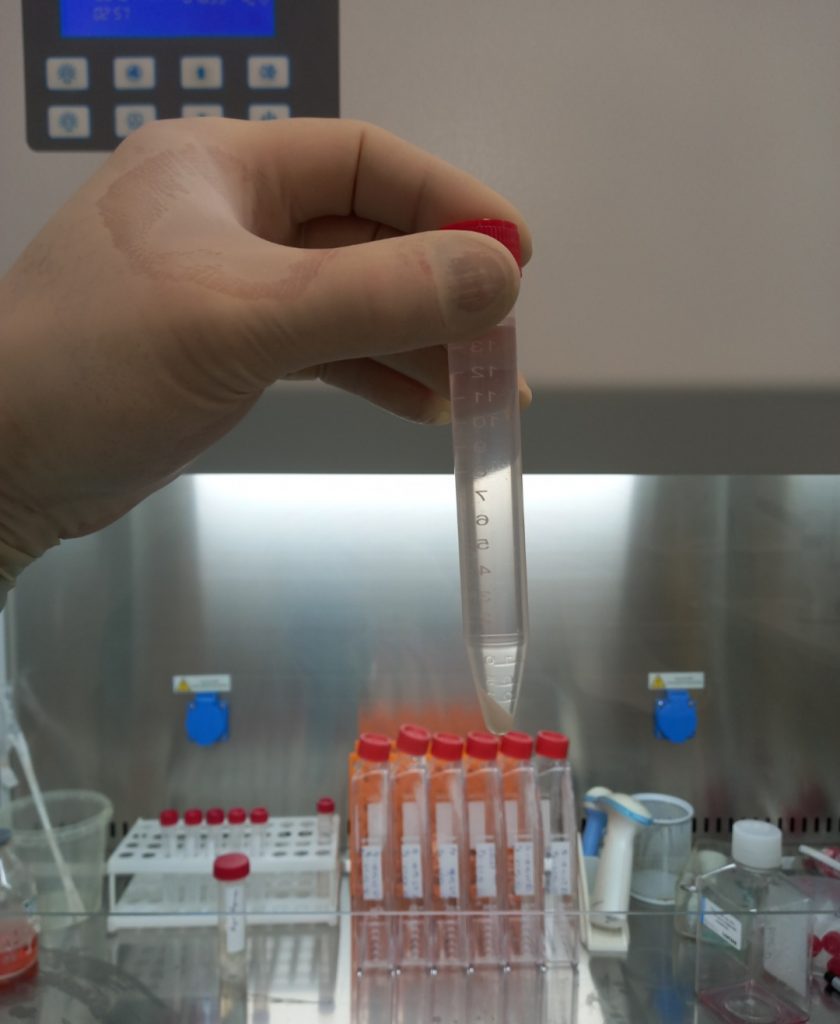
How is Primary Cell technology different from other stem cell therapies?
Primary Cell is a fast, inexpensive, effective, and safe method of treatment and rejuvenation with suspensions of their own signal cells, the mesenchymal stem cells, pericytes, fibroblasts, macrophages that are released from a small amount of adipose tissue of 25-40 milliliters. At the same time, the technique of fermentation, washing, and passage without a stage of long cultivation is applied.
Cells are injected locally by the method of peptide activation of regenerative and proliferative processes in tissues.
Advantages of Primary Cell technology:
• Biosafety – the absence of a long cultivation period minimizes the risk of infection and mutations.
• Significant clinical effect in comparison with intraoperative technologies of insertion of stem cells from adipose tissue (in which there is no laboratory stage of cultivation).
• Low-trauma procedure. Only 40 -25 ml of adipose tissue (lipoaspirate) is enough for the course of treatment
• Painless and short-lived mini liposuction procedure performed under local anesthesia.
• Attractive price due to optimized processing cycle, which does not require a large number of reagents and culture vessels for extraction and scaling of cellular material.
The technology of laser routing of cellular autografts
The innovative technique of laser routing of cellular autografts provides active stimulation of regenerative processes of human tissue and their rejuvenation by exposure to the medical fractional CO2 laser beam with a diameter of 120-300 μm with a wavelength of 10.6 μm.
The technology involves the introduction (infiltration) into the skin of a tissue suspension based on active fibroblasts and platelets (plastic, cell-tissue material) to ensure enhanced tissue regeneration and rejuvenation. The suspension is injected along the lines of action of the medical fractional CO2 laser on facial tissues.
The use of tissue suspension based on active fibroblasts and platelets slows down the aging process, increases skin tone, and starts the process of rejuvenation of local tissues and the body as a whole. The suspension activates the cells of the facial skin due to the body’s own reserves and triggers the biological mechanism of natural rejuvenation without surgery and other radical measures.
Active fibroblasts locally stimulate regeneration, enhance the process of collagenosis, osteogenesis, and angiogenesis, improve blood circulation and intercellular metabolism, as a result of which the body, at the cellular level, begins to function again in youth. Accelerates the synthesis of collagen, elastin, and hyaluronic acid, which restores and returns youth and elasticity of the skin.
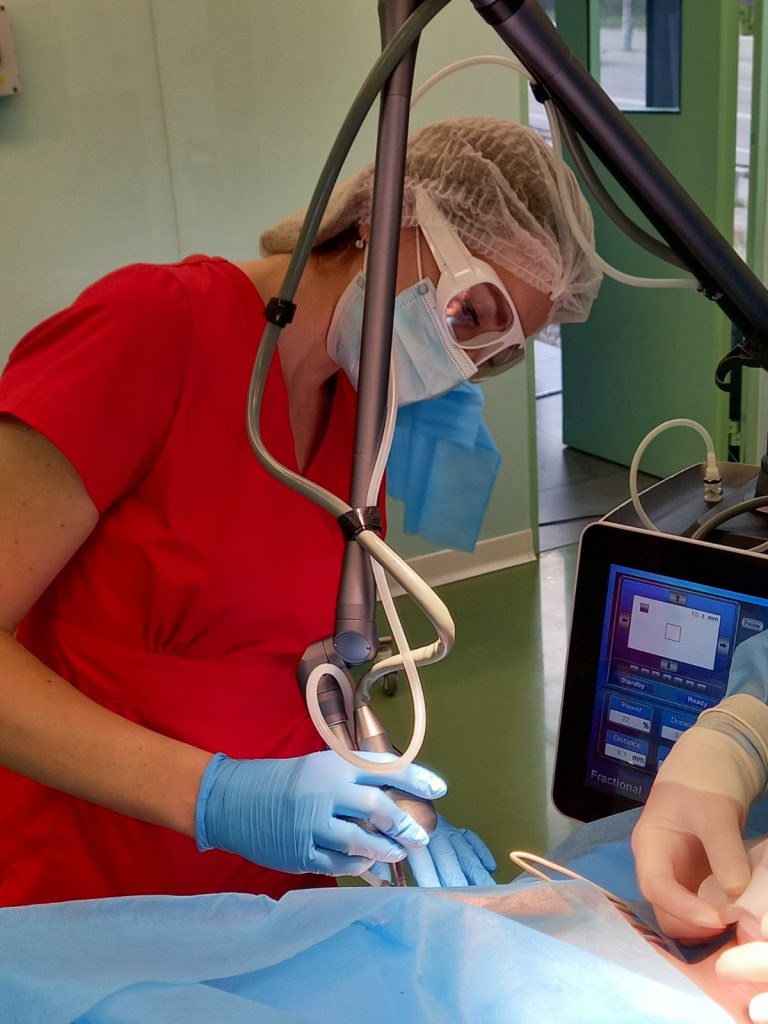
Effects of the procedure:
• improving skin color
• reduction and straightening of facial wrinkles
• improving skin metabolism
• increase skin tone and elasticity
• inhibition of aging processes
• moisturizing the skin and restoring water balance
• accelerate skin regeneration
• treatment of acne and post acne
• removal of pigment spots
• accelerating skin rehabilitation after peels
In turn, the use of medical fractional CO2-cosmetic lasers helps to restore the structure of the skin, helps eliminate wrinkles and narrow enlarged pores of the skin. Beams of light of different lengths penetrate the epidermis without damaging its upper layers. The fractional laser causes microdamage to the skin at a depth of 1.5 mm, stimulates collagen production and regeneration.
Collagen fibers are reduced by 1/3 of the length, which increases the elasticity of the skin, tightens the skin, and significantly reduces wrinkles. Thus, the laser beam penetrates the skin, which leads to rapid heating of the tissues, because it is the thermal effect that is the trigger to start the recovery process.
The method is carried out as follows:
Facial skin, areas of which need to be rejuvenated and stimulated (accelerated) regeneration processes are treated with a medical fractional CO2 laser with a diameter of 120-300 μm and a wavelength of 10.6 μm, followed by 15-30 min, intertissued insertion of cell suspension based on active fibroblasts and platelets.
Thus, the method of laser routing of cellular autografts has a number of advantages over the known, because the introduction of tissue-cell suspension based on active fibroblasts and platelets along the lines of impact of fractional CO2 laser on facial tissues allows, due to plastic material, to provide resources for enhanced regeneration and regeneration of the tissues, to effectively stimulate regenerative processes in tissues, prevention of age-related changes in the underlying tissues and the body as a whole.
Hydrogel scaffold is the regenerative wound coating
The regenerative bandage has been used successfully to treat trophic ulcers and burns. The wound coating has also been used as a matrix carrier for cell grafts, biologically active substances, growth factors, and antiseptics.
The innovative regenerative agent consists of a polyester mesh that retains on its surface a hydrogel substance represented by hyaluronic acid and sodium alginate. The multifunctional hydrogel complex allows to successfully transfer cultured in vitro fibroblasts to the wound surface, similarly, the tool has been tested for delivery of mesenchymal stem cells to the wound surface, which effectively accelerates the regeneration and healing of trophic ulcers, burns, and other skin lesions.
The regenerative agent has been successfully clinically tested as a carrier bandage for epidermal growth factor in combination with antibiotics, which makes it possible to treat chronic wounds and defects with slow regeneration in patients with weakened immune systems.
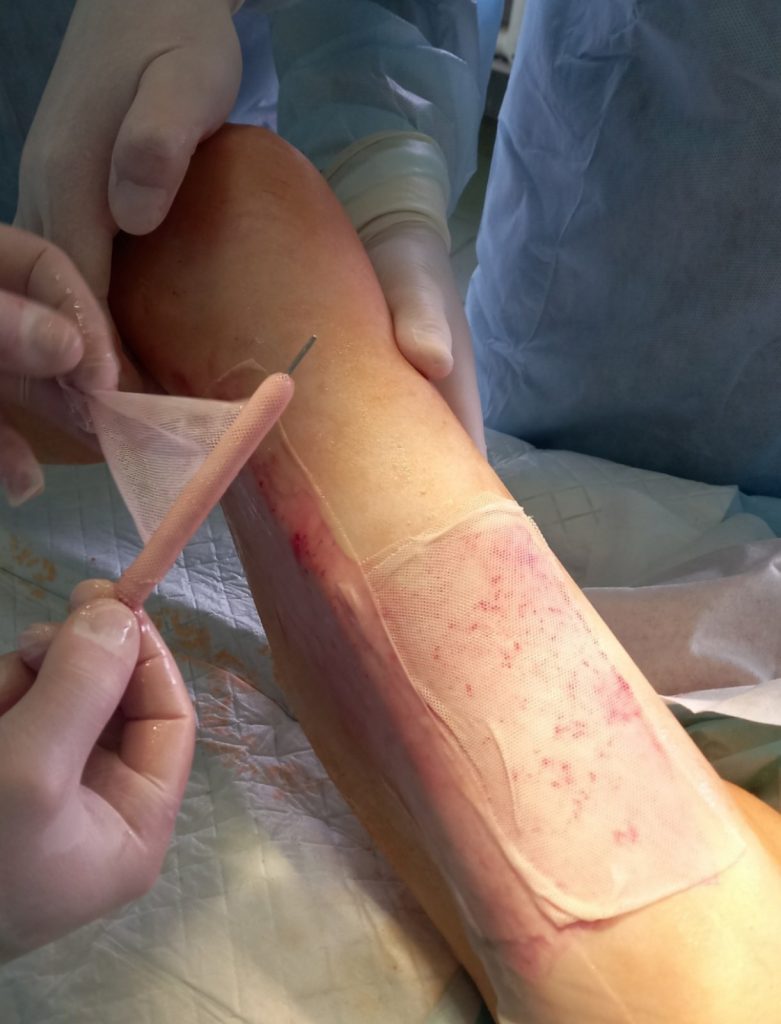
Modified punch dermoplasty with transplantation of cultured autofibroblasts
One of our innovative solutions is a minimally invasive method of skin transplantation using cultured autofibroblasts.
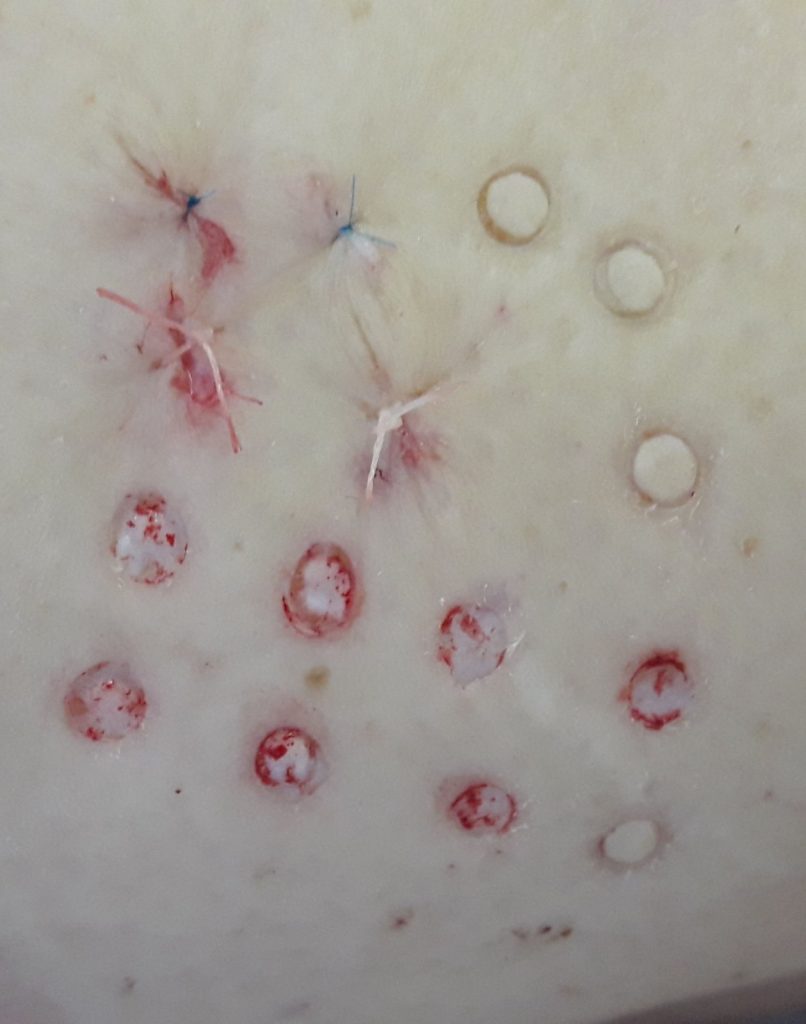
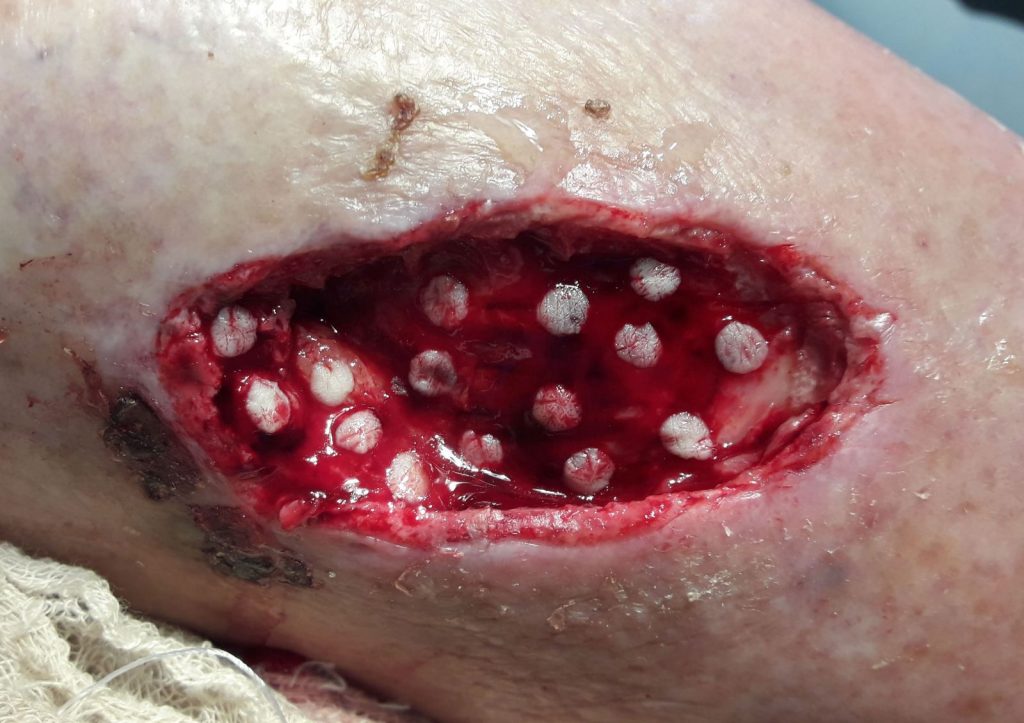
The method is effectively used for the surgical treatment of patients with post thrombophlebitic ulcers of the lower extremities. The collection of donor autodermotransplants is performed on the lateral surface of the thigh with the help of a punch – a surgical cutting instrument made in the form of a tube with a diameter of 3 or 4 mm. On the surface of the skin of the thigh, there is a “drilling” of dermal microfibers of appropriate diameter (3 or 4 mm), 0.4-0.8 mm thick, and the donor bed is sutured with a nodal or intradermal micro steam. Subsequently, punch dermal grafts are fixed on the surface of the granulating wound at a distance of 1-1.5 centimeters from each other. Injections of resuspended fibroblasts are performed under each micro flap, in a ratio of 500 thousand cells per 0.5 milliliters of saline. The introduction of cell suspensions is carried out for 1-5-10 days after punch dermoplasty.
The study of planimetric indicators of the wound surface revealed the activation of reparative processes when using autodermoplasty in combination with injections of resuspended fibroblasts, which prevents secondary infection of the wound, reduces the duration of treatment and hospital stay. And the use of autotodermoplasty by the punch method and injection of resuspended fibroblasts – islet (injection was performed under each micro flap) allows for outpatient treatment, which significantly mixes the cost and increases compliance with patients.
Pneumatic helmet
Portable respiratory protection system with positive airflow
At the initial stage, the concept model of a pneumatic helmet was developed in order to protect employees of biotechnological laboratories from dangerous biological agents (infectious agents – viruses, bacteria) and toxic agents. However, in the midst of the COVID-19 coronavirus pandemic, the purpose of the helmet has become different, in a more global scope. Thus, in order to effectively protect against dangerous infectious agents, including coronavirus, a team of scientists from Ternopil I. Gorbachevsky National Medical University (TNMU) and the “Genom” team developed a unique prototype of a mobile respiratory protection system with forced airflow (concept model of a pneumatic helmet), which has no analogues in the world.
The project of development of the innovative system of respiratory protection of respiratory organs included the following tasks which managed to be realized:
Development and improvement of the system of forced air supply, which creates laminar protection with filtered, purified air of the respiratory organs and skin of the head and neck. Providing a system of portable mobile long-term power supply with the possibility of “hot” battery replacement. Creating a system of forced air supply in the pneumatic helmet through the use of a compact, ergonomic turbine with its own filter and low noise source. Development of a multi-component air intake filtration system with a pneumatic helmet. Creating a semi-closed circuit of the pneumatic helmet with an active supply of purified air and forced displacement of user exhaust air. Ensuring optimal visual inspection with a panoramic viewfinder mounted in a semi-closed contour of the helmet.


